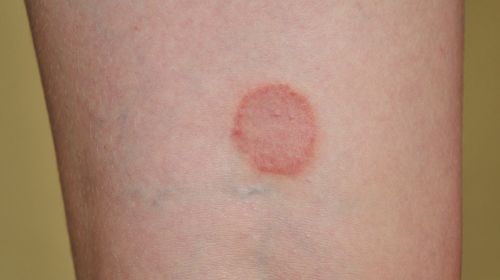
Lichen sclerosus is a chronic skin disease that mainly occurs in the genital area. The skin disease is not curable and can lead to serious consequential damage if left untreated. Appropriate therapy and compliance with rules of conduct can help.
- The chronic skin disease lichen sclerosus mostly occurs in the genital area – more often in women.
- © iStock.com/Doucefleur
Lichen sclerosus can affect men and women of all ages, and in rare cases even children. However, adult women are most often affected.
The skin disease is not contagious, but affects those affected with severe inflammation, itching, soreness and the formation of white spots and nodules. With suitable and early therapy, the symptoms can be significantly reduced and complications avoided.
Overview of article content:
How is lichen sclerosus treated?
The best way to treat the symptoms of lichen sclerosus is with cortisone therapy. The following treatment regimen has been established:
Acute treatment for lichen sclerosus
Three-month steroid shock therapy with highly potent glucocorticoids that have to be applied daily. Studies show that this treatment significantly improves symptoms in 75 to 90 percent of those affected. In the case of very pronounced symptoms such as severe itching or pain, the therapy can be combined with intralesional glucocorticoid injections (injections into the affected skin areas).
This is followed by a so-called skip phase, in which only nursing measures are used. If there is a recurrence (recurrence of the symptoms), reduced glucocorticoid shock therapy is carried out over a week and then an attempt to leave is started again.
A medicinal alternative is treatment with calcineurin inhibitors (tacrolimus and pimecrolimus). With these ointments and creams there is less thinning of the treated skin, but the potency is not as high as with glucocorticoids. In young women, for whom the symptoms are only very slight, treatment attempts with creams containing estrogen and progesterone can also be successful.
No meaningful studies are available on the success rates of cryosurgical measures (icing). Photodynamic therapy (light therapy) seems to achieve positive results in lichen sclerosus in the female genital area.
Follow-up treatment and rules of conduct for lichen sclerosus
Many women – especially those with anogenital lichen sclerosus – require years and sometimes life-long treatment.
In addition to permanent ointment treatment with a medium-strength steroid twice a week, special skin care and general rules of conduct are in the foreground:
meticulous intimate hygiene (use of a bidet or cleansing oil wipes, little soap)
daily skin care with greasy ointments without fragrances
before sporting activities or long marches, apply a protective ointment (e.g. petroleum jelly)
Silk linen is preferable to cotton
Avoid mechanical skin irritation from hard toilet paper or towels, damp toilet paper, hard bicycle saddles and tight clothing
In men, especially in the case of uncomplicated forms of the anogenital course, the full circumcision (removal of the foreskin) should be carried out in the early stage.
What is a lichen sclerosus?
The lichen sclerosus ("lichen" from Greek "leichen" = lichen, "sclerosus" from Greek "scleros" = hard, dry, brittle) is an inflammatory skin disease in which it develops into whitish, coarse, slightly raised spots and in the advanced stage of the disease There are skin knots that can fuse and remind of scar tissue. The skin changes are benign and are not triggered by an infection or an allergic process.
If left untreated, the lichen sclerosus can lead to scarring, sticking and shrinking of skin areas that can no longer be reversed and there is a slightly increased risk of malignant skin changes in the affected area.
Lichen sclerosus is caused by chronic inflammation of the connective tissue in the dermis. The symptoms appear mainly in the area around the anus and the external genital organs. Only in about 20 percent of cases does the skin disease manifest itself outside the genital area, for example under the breast, in the back-shoulder region or on the inner thighs.
On the basis of the regions affected, a distinction is therefore made between the anogenital (in the anal and genital region) and the extragenital (outside the genital region) lichen sclerosus. One then speaks of the lichen sclerosus genitalis and extragenitalis. In contrast to the anogenital form, the extragenital form of the lichen sclerosus usually occurs asymmetrically.
Another classification is based on the age at which the disease occurs: Before puberty, one speaks of "prepubertal", then of "post-pubertal" lichen sclerosus.
The disease can occur at any age and in both sexes, but women are affected about ten times more often than men. Lichen sclerosus is most often diagnosed in women after the menopause (postmenopausal), but the symptoms begin much earlier in half of these women.
Children (0.3 percent of cases) and women older than 80 years (three percent) are least likely to fall ill. These old women are almost all immobile (bedridden) at the beginning of the disease and have urinary incontinence. A high number of unreported cases is suspected, since the skin disease is accompanied by no or very little symptoms in ten percent of cases and, on the other hand, a certain percentage of those affected do not see a doctor despite complaints, often out of shame.
Symptoms of lichen sclerosus
One of the most distressing and early symptoms of the disease is persistent or seizure itching. In the area of the affected skin, the inflammation leads to redness, later to rough, white spots and nodules, which can converge to form larger areas (plaques). Over time, the skin thins out (atrophy) and there are painful tears and bleeding, later typically also scarring.
With the extragenital course, the affected skin can be discolored (depigmented) and blistering sometimes occurs. Anogenital and extragenital courses can occur in parallel.
The anogenital course is different in men and women.
Women: In women, itchiness and reddening of the skin in the area of the clitoris often appear first. The skin changes then spread to the entire vulva, especially the inner and outer labia and the area around the anus and perineum. The mucous membranes are typically left blank, which often results in the characteristic shape of an eight. Clitoris and small narrow lips can stick together and the tissue around the vaginal entrance can shrink, both of which contribute to narrowing the vaginal entrance. Sexual intercourse can become very painful and uncomfortable, and skin tears and bleeding can occur.
Men: In men, lichen sclerosus is most common on the glans and foreskin, less often on the perineum. The skin change can result in narrowing of the foreskin or hardening of the skin in the area of the glans. Both lead to the fact that the foreskin can no longer be pushed back or only with difficulty, which complicates intimate hygiene and can trigger a chronic inflammation of the glans skin (balanitis). The skin tears easily, which is also painful, can cause erectile dysfunction and can severely hinder sexual intercourse.
Both genders: Lichen sclerosus can make bowel movements difficult and cause constipation due to the strong itching and painful skin tears in the anal area. Pain may also occur when urinating, and if the illness is long, there may be a scarred narrowing of the urethra, which may weaken the urinary stream.
Causes and Risk Factors of Lichen Sclerosus?
The exact cause of lichen sclerosus is still unclear. According to the current state of knowledge, it is only certain that the disease is not contagious or sexually transmitted. However, studies indicate that various factors could be involved in the development of the disease:
Genetic predisposition (predisposition)
At least ten to twelve percent of those affected have relatives who also have lichen sclerosus. Due to the high number of unreported cases, the proportion of sick blood relatives is even significantly higher.
Autoimmunological process
The damage to the skin barrier by the lichen sclerosus could also be caused because cellular proteins become vulnerable to the immune system and this triggers an immune response against the body's own tissue (autoimmune reaction). In addition, oxidative DNA damage and TP53 mutations were detected in many samples from infected tissue, which could also indicate an autoimmune background.
It is particularly striking that the proportion of women who suffer from lichen sclerosus and at the same time from another autoimmune disease is very high at 30 to 50 percent. This also indicates a connection.
Hormones and lichen sclerosus
At least in women affected, it can be seen that lichen sclerosus mainly occurs outside the fertile phase of life. Estrogen levels are low in girls before puberty and in women after menopause. Most cases of lichen sclerosus occur in these phases of life. Female sex hormones seem to partially prevent the development of the disease. This assumption fits that post-menopausal hormone replacement therapy or contraception with progesterone have a certain protective effect against the disease.
In addition, a lower level of the male sex hormones testosterone and androstenedione is found in skin lesions in women with lichen sclerosus. Both are involved in the regulation of skin growth in the area of the genital organs and are probably linked to the development of lichen sclerosus. This would also explain why, in one study, women who took an antiandrogenic contraceptive such as chlormadinone acetate, cyproterone acetate, dienogest or drospirenone had a significantly higher rate of lichen sclerosus.
Trauma as the cause of lichen sclerosus
There are certain triggers that play a role in the development of disease-specific skin changes in the lichen sclerosus. Scratching and rubbing (e.g. through tight clothing) can trigger the anogenital and also the extragenital form.
In the anogenital form, surgical interventions (for example, loosening a foreskin bond), births, injuries to the external genitalia due to accidents or sexual abuse and tears in the foreskin during phimosis are triggers for the onset of the disease. In addition, it is discussed whether the lower mucus production in women after the menopause leads to increased friction on the genital organs, which injures the skin and thus favors lichen sclerosus.
Associated diseases
In addition to autoimmune diseases, there are other diseases that are common in people with lichen sclerosus. There are differences between men and women.
The following diseases occur frequently in sick women:
In men you can find:
Medicines that cause lichen sclerosus
There is evidence that some medications (carbamazepines, imatinib) can cause lichen sclerosus.
How to diagnose lichen sclerosus
A doctor can generally suspect the presence of lichen sclerosus by taking a medical history and looking at the affected skin regions. The combination of whitish skin changes and itching (especially in the anogenital area) is a clear indication of lichen sclerosus.
However, there are a large number of similar-looking diseases that must be excluded. For this purpose, the doctor takes a biopsy (skin sample) in the area of a skin change under local anesthesia, which is examined by specialists under the microscope. The following suspected diagnoses must be excluded:
- bacterial infections
- malignant skin changes
- Fungal infection (Candida infection)
- Lichen planus
- Vitiligo (white spot disease)
- atopic eczema (neurodermatitis)
- Psoriasis
Course of the disease and prognosis
Lichen sclerosus is a chronic disease that has a slowly progressing tendency. According to current knowledge, a cure is not possible. There is a low rate of spontaneous improvements, especially in young girls, which, however, rarely lead to permanent freedom from symptoms, because symptoms usually appear again in adulthood.
Consistent treatment with strong glucocorticosteroids can at least suppress the symptoms in 75-90 percent of the women affected and 90-100 percent of the men. After the initial shock therapy, low-dose cortisone therapy and careful compliance with the behavioral rules are usually sufficient. However, those affected are not cured and a trigger – but also without an understandable reason – can worsen the symptoms at any time.
Existing scarring does not regress in the course of therapy, but early treatment reduces the risk of scarring and carcinoma development.
Carcinoma risk slightly increased in lichen sclerosus
People with anogenital lichen sclerosus have a slightly increased risk of developing squamous cell carcinoma in the genital area. This is not the case with the extragenital course. Consistent long-term treatment seems to significantly reduce this risk. As part of long-term therapy, a medical check-up should be carried out every six to twelve months in order to detect cell changes in good time.
Psychosocial consequences from lichen sclerosus
An active lichen sclerosus significantly influences the quality of life. In addition to the physical symptoms, feelings of shame burden those affected. There are restrictions in social activities because clothing must be selected accordingly, sports can only be carried out to a limited extent and hygienic and nursing measures can only be followed with difficulty on the way. Pain during intercourse leads to a significant restriction of sex life in both sexes.
Can you prevent lichen sclerosus?
One can try to avoid injuries and damage to the skin (especially in the genital area) in order to reduce the trigger effect. For this reason, those affected should refrain from clothing that is too tight, too frequent washing of the genital area with soap, hard towels and hard toilet paper, vaginal rinses, wet wipes and sports such as riding or cycling. Careful skin care with suitable products can also help prevent it. There is no experience of whether a certain diet affects the disease.