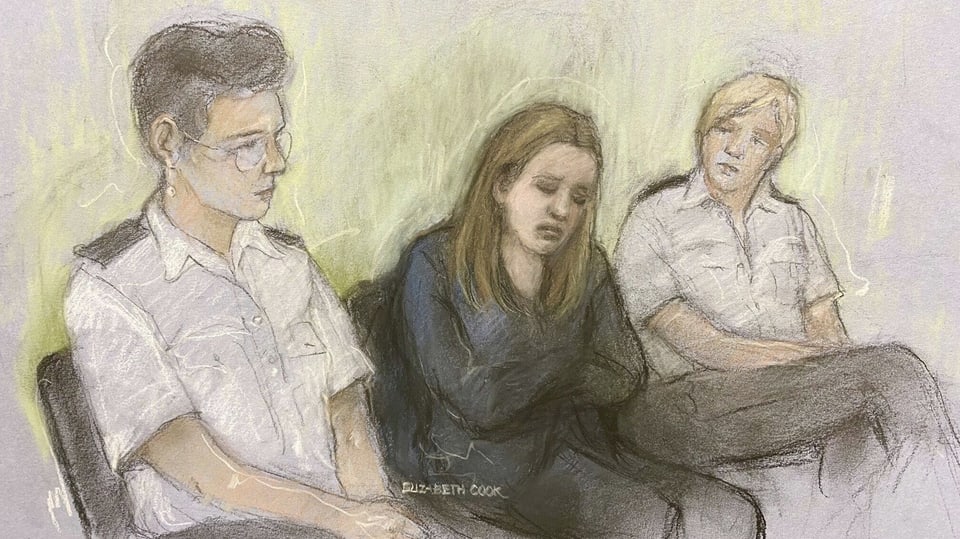Contents
The case of a child murderer roils the kingdom. In Switzerland, too, nursing staff have already become perpetrators – the institutions are trying to minimize the risk.
“You acted cruelly, calculatedly and cynically, and coldly denied any responsibility for your actions. Only a sentence of life imprisonment comes into question for a just punishment »: With these words the judge turned to the accused. He then read the verdict: “Lucy Letby, I convict you of all seven counts of murder.”
The case is currently stirring up the whole of Great Britain. The former nurse has been convicted of crimes beyond imagination: she killed seven babies and tried six others at a hospital in northern England.
The motive for the atrocities remained open at trial. The 33-year-old denied the crime until the end. She stayed away from the verdict.
Legend:
Letby is only the fourth woman in Britain to be sentenced to the maximum sentence known as the “whole life order”. Two are in custody, the third died behind bars.
Keystone/AP/Elizabeth Cook
Patients entrust their lives to medical professionals. When this “God is playing,” as the prosecutor put it in court, it is the ultimate betrayal of trust – in the institutions as a whole.
Cases like the one in England have happened time and time again throughout history. The “angels of death from Lainz” are notorious: in the 1980s, four ward workers killed dozens of people in a hospital in Vienna. In the US, nurse Charles Cullen confessed in 2003 that he murdered up to 45 patients over 16 years. In Germany, the so-called “death nurse” was convicted of 85 murders in 2015.
Look instead of looking away
At the beginning of the millennium, Switzerland was shaken by the case of the “death nurse from Lucerne”. Between 1995 and 2001 he murdered in nursing homes in central Switzerland. His victims: At least 22 elderly people in need of care.

Legend:
The “death nurse from Lucerne” poisoned or suffocated his victims. As a motive he gave overload and pity. He is still serving his life sentence.
Keystone/Linda Graedel
But how can homes and hospitals prevent the staff from causing suffering to those in need of protection for years and even killing them with impunity? There are safety precautions and automated processes to minimize the risk, explains Yvonne Ribi, the top nurse in Switzerland.
It is also important that there is a culture in every team that anomalies are reported to the superiors. Suspicions must be taken seriously. And that at all hierarchical levels. This is also expressed in the charter of the home association Curaviva, which says: “We’re looking!”

Legend:
In the case of Lucy Letby, people obviously looked the other way: For years, information was ignored – including by the hospital management, who feared an investigation that would damage their image.
Keystone/AP/Jacob King
However, prevention begins during training, says Ribi. “Carers are very well trained professionals – and that is also very important.” Mistakes and misuse can have fatal consequences. Anyone who administers medication or infusions bears a great deal of responsibility. It is therefore important in training to address this risk potential.
The conditions must be created so that caregivers can do their work to the best of their knowledge and belief.
Technological progress also helps to prevent abuse, says Ribi: “If, for example, morphine is administered, it will be fully registered if the institution has such systems.” In addition, the four-eyes principle must be applied to drugs with a particular risk potential. “It’s part of the operational standards.”
Ribi is convinced that the nursing staff in Switzerland would do everything possible to guarantee the integrity of the patients and residents. Ultimately, however, she also sees politics as having a duty to avoid mistakes caused by stress and overload: “The conditions must be created so that caregivers can do their work to the best of their knowledge and belief.”