Author: Jan Groh, medical writer
Last update:
March 16, 2021
Sickle cell disease is rare in Northern Europe. Those affected suffer from anemia and circulatory disorders. The hereditary disease requires lifelong treatment.
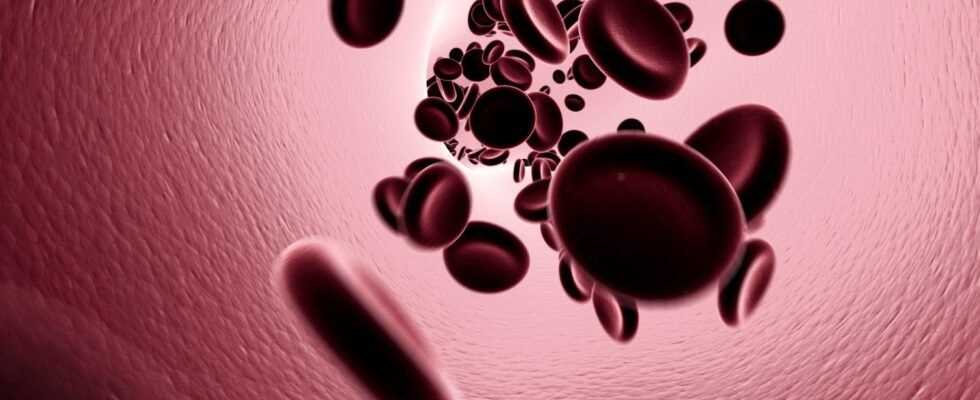
- In sickle cell amemia, the red blood cells, the erythrocytes, are deformed.
- © Getty Images / iStock.com / FFormat
Doctors refer to all diseases as sickle cell diseases in which a specific red blood pigment known as HbS occurs that deviates from the norm. The cause of these diseases is a change in the genome of those affected, which means that the red blood pigment – hemoglobin – tends to clump together.
Article content at a glance:
Forms, distribution and frequency of sickle cell anemia
Doctors differentiate between different forms of sickle cell disease. The earlier than Sickle cell anemia and today as Sickle cell disease The most severe form of disease referred to is present if both parents inherited an HbS system. Mixed forms with other hematopoietic disorders can also occur, including the severe sickle-cell beta-thalassemia, in which one parent inherits the predisposition for HbS and the other the predisposition for thalassemia.
Sickle cell disease is very rare in Europe. According to estimates, the number of people affected in Germany is up to 1,000. The genetic make-up for sickle cell disease is more common in Africa, Latin America, Asia and the eastern Mediterranean. This distribution coincides or coincided with the distribution area of malaria until the modern fight against the disease. Since people who inherited the HbS system from only one parent have a natural protection against malaria, the genetic make-up had proven to be a survival advantage in the distribution area of the tropical disease, although carriers of maternal and paternal HbS systems died early from sickle cell disease.
Typical symptoms of sickle cell disease
Due to the typical changes in the red blood pigment, the red blood cells (erythrocytes) are less easily deformable and change from the normal, rounded, indented shape to a sickle shape, especially when the oxygen content in the blood is low. Both the lower deformability and the sickle shape prevent the red blood cells from sliding in the blood vessels. If the blood cells get stuck in the narrow blood vessels, they prevent the tissue from being supplied with oxygen and nutrients. The result is circulatory disorders.
Sickle-shaped red blood cells also tear easily and die prematurely. In addition, the spleen recognizes them as defective and holds them back so that they are no longer available for oxygen transport.
To the Symptoms of sickle cell disease belong:
- Anemia
- fever
- Repeated pain crises in the affected body regions (including often bone pain) as a result of circulatory disorders
- Jaundice due to the increased breakdown of red blood pigment
To the serious complications belong:
- "Spleen sequestration": some or almost all red blood cells sink into the spleen within a few hours; the result is a state of shock
- "Acute Thoracic Syndrome" (ATS): Chest pain, cough, shortness of breath, and fever similar to pneumonia
- stroke
- "Priapism": painful permanent erection that can damage the erectile tissue of the penis and lead to the inability to conceive
- High blood pressure in the lungs
Age of onset: when do symptoms appear?
Some of the red blood pigment in the blood of small children has a different composition than in later life. This so-called fetal hemoglobin is not influenced by the genetic change that leads to sickle cell disease. The first symptoms of the disease therefore only show up from around six months of age, when the proportion of fetal hemoglobin has decreased significantly.
For this reason, sickle cell disease is usually diagnosed in childhood after six months of age. In the case of less severe forms of the disease, symptoms and a final diagnosis can only arise in adulthood.
Diagnosis of sickle cell disease
The typical complaints together with the mostly southern origin of those affected provide first indications of the presence of the disease. The exact diagnosis is made based on blood tests and analysis of the red blood pigment. In addition, the doctor examines the extent to which the disease has already caused damage to the skeletal system, especially the hip bones, and to other organs such as the lungs, heart or eyes.
Treatment options
The only therapy that can completely cure sickle cell disease is bone marrow or stem cell transplantation. Due to the risks associated with the treatment, which exist as a result of the transplant preparation, especially for adult patients and which can extend to death, stem cell transplants have only been carried out in a few, mostly very young, patients worldwide.
Other treatments for sickle cell disease aim to relieve existing symptoms, prevent infections, and prevent pain attacks. A large number of measures and drugs are used.
Blood transfusions are only carried out in exceptional cases, despite the often very low levels of red blood pigment in the blood. Because the attempt to achieve "normal" blood values in those affected can lead to serious complications due to the poor flow properties of the sickle cells.
Prognosis: life expectancy with sickle cell disease
In Europe and the United States, around nine in ten children with sickle cell disease will reach adulthood. However, the life expectancy of those affected is also shortened in the industrialized countries. The average life expectancy with optimal medical care is around 50 years. Apart from the limitations caused by an acute illness, the patients can lead a normal life.
A desire to have children can also be fulfilled. To prevent sickle cell disease from being transmitted to the child, it is possible to have a tissue sample taken from the placenta and examined between the tenth and twelfth week of pregnancy. If it turns out that the fetus is affected by the genetic change, the pregnancy can be terminated at this point at the request of the parents. The so-called pre-implantation diagnosis, with the help of which the genetic properties of an embryo created by artificial insemination can be determined before implantation in the womb, is forbidden in Germany.